Cystoscopy
Procedures we perform
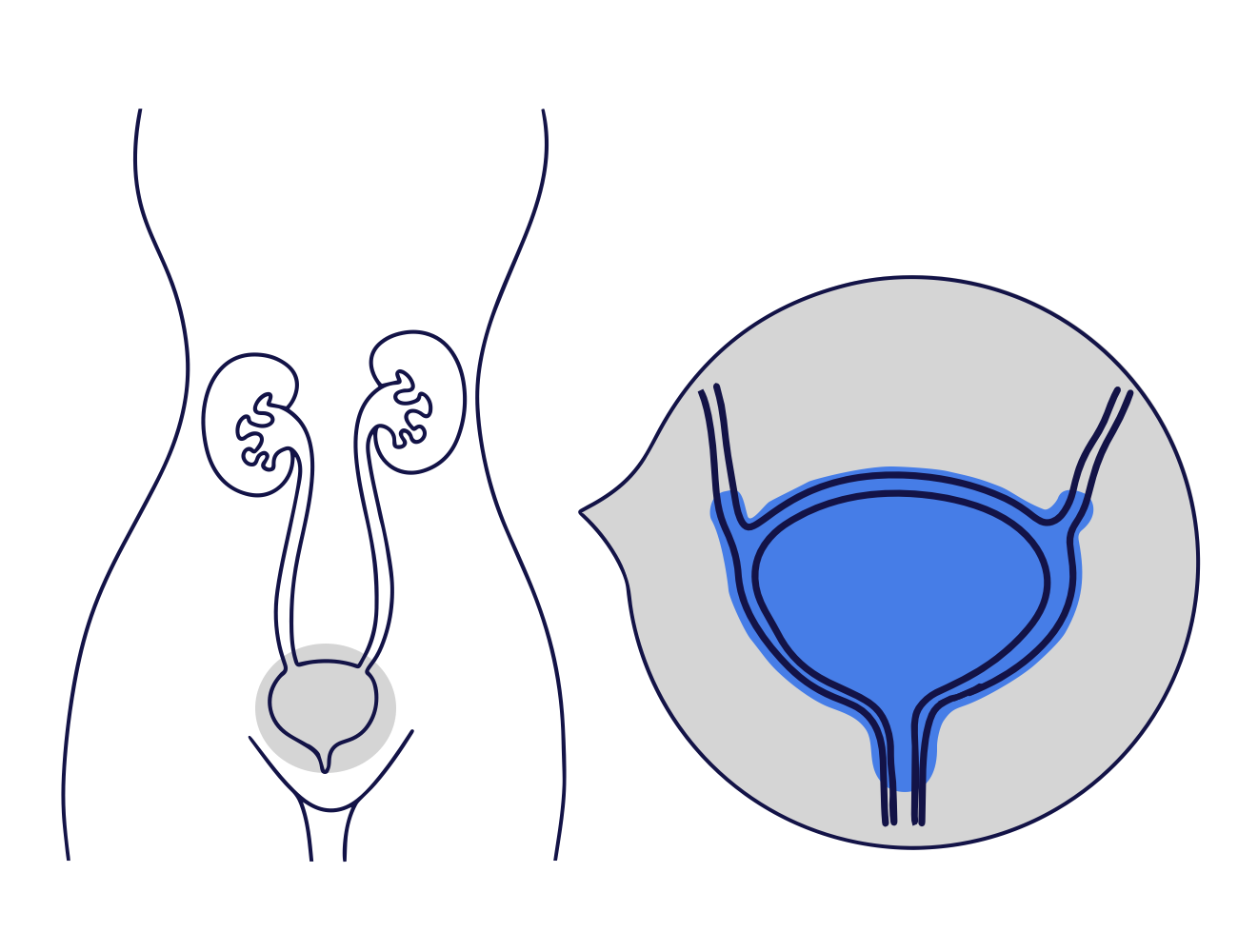
ABOUT CYSTOSCOPY
What is a cystoscopy?
A cystoscopy is a procedure to look into the bladder by passing a telescope through the urethra (the tube you pass urine through).
Why is a cystoscopy required?
Cystoscopy is performed to investigate and treat problems with the bladder and the urethra.
Common reasons for a cystoscopy include:
Blood in the urine.
Recurrent urinary tract infections.
Urinary symptoms such as frequency, urgency, incontinence, and difficulty voiding.
Bladder cancer.
Bladder pain.
Urethral stricture.
Read more about the conditions requiring cystoscopy below.
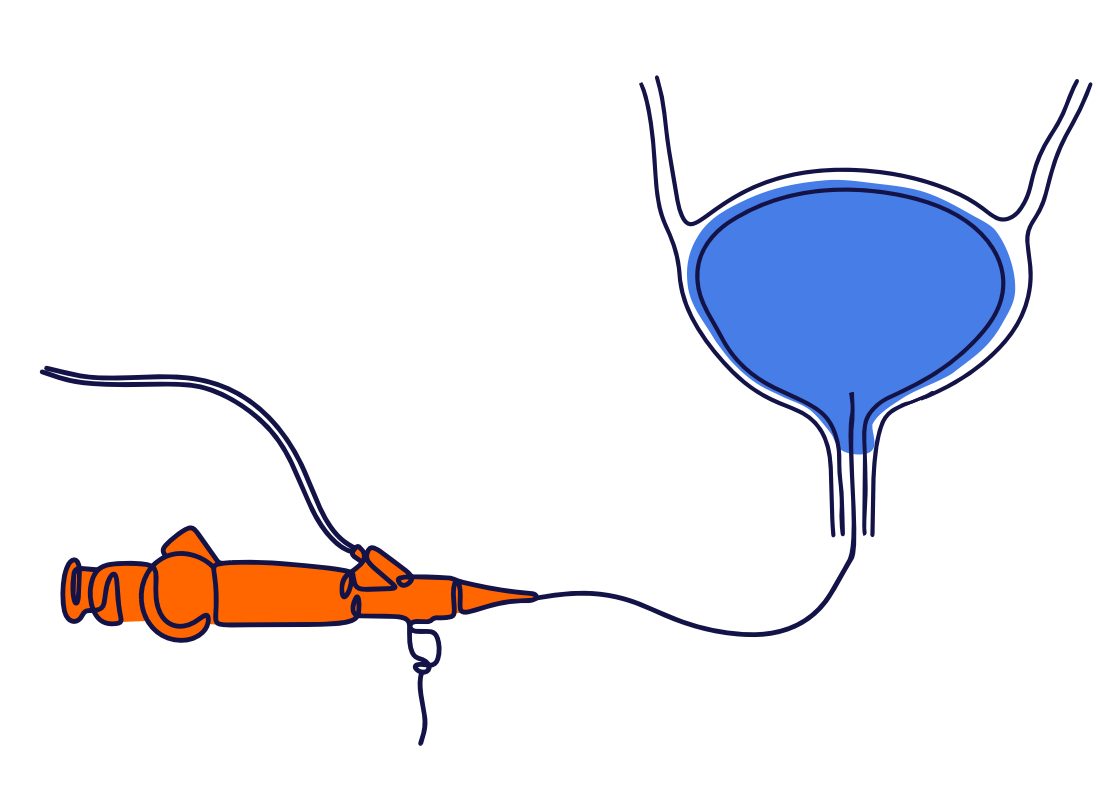
PATIENT JOURNEY
OUR TEAM
Meet our Urologists
All of our Urologists perform cystoscopy. Click on the links below to learn more about our doctors.