Bladder Botox
Procedures we perform
ABOUT BLADDER BOTOX
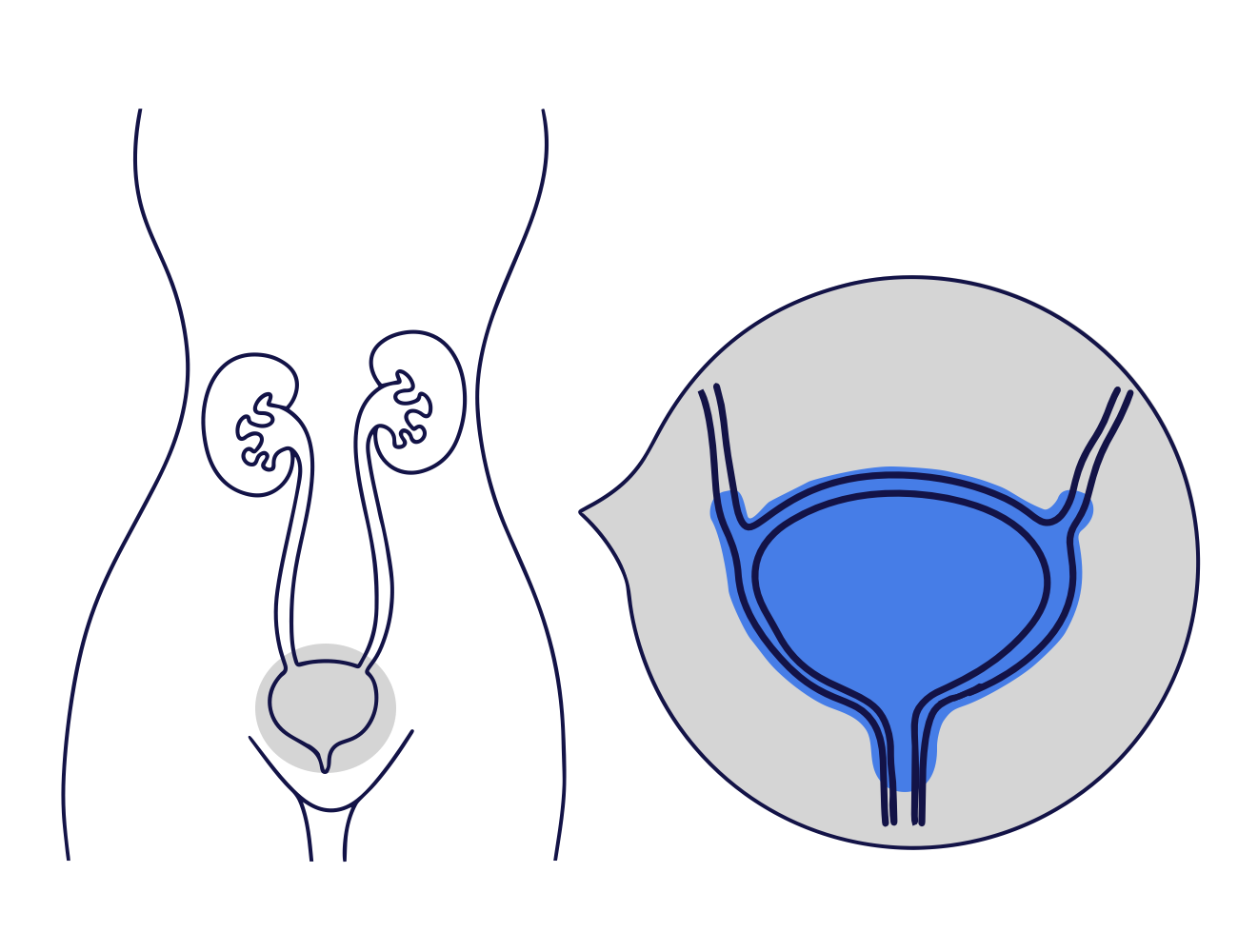
What is Bladder Botox?
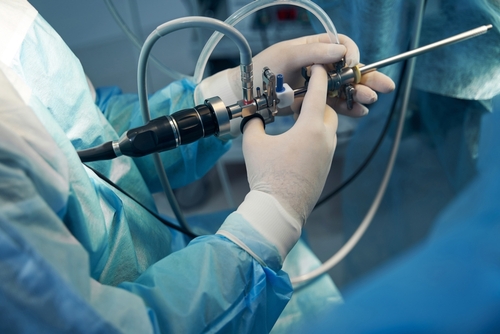
Bladder Botox, also known as Intravesical Botox, is a procedure to inject the muscle relaxant botulinum toxin (Botox) into the bladder wall.
It is performed by passing a telescope through the urethra (the waterpipe) into the bladder, known as a cystoscopy.
Why is Bladder Botox required?
Botulinum toxin (Botox) is a muscle relaxant which works by temporarily reducing the ability of the bladder wall muscles to contract (squeeze).
Bladder Botox is most commonly used to treat urinary symptoms due to Overactive Bladder (OAB), including:
Urinary frequency
Waking at night to pass urine
Urinary urgency
Urinary incontinence
Read more about urinary incontinence below.
PATIENT JOURNEY
OUR TEAM
Meet our Urologists
The following Urologists in our practice perform Bladder Botox: